Meeting the physiotherapist
In outpatient clinics or during your hospital stay, you will meet a physiotherapist who will teach you techniques to clear your child's chest to prevent a build up of secretions which, if left, can lead to chest infections.
Airway clearance
These techniques will be reassessed regularly at each clinic visit and modified as necessary by the specialist PCD physiotherapist to ensure your child is getting the best treatment. Babies and toddlers will be dependent on parents to help them but, as they grow, it is our aim that your child will be independent with their physio when they are old enough.
Each patient will have a physiotherapy routine that is tailored specifically to their needs. Please let the physiotherapist know if you are having problems.
Babies and infants
Parents should be taught modified gravity-assisted positions and intermittent chest clapping. Positions should include:
- Sitting until approximately six months of age to drain the top of upper lobes of both lungs (once upright and more mobile these areas drain easily),
- Lying on the back (to drain the front of the upper lobes of both lungs)
- Alternate side lying (to drain the lower and middle lobes).
Intermittent percussion should be performed for 30 second intervals using a cupped hand or few fingers (depending on the size of your child and your own hands) and over a towel for comfort. It should be performed before a feed or at least 1 hour after feeding.
Baby exercises and jumping and blowing games should be introduced as early as possible.
There are other techniques such as infant PEP and Assisted Autogenic Drainage and these will be introduced by your physiotherapist if appropriate.
Two to four years and upwards
Parents should continue with intermittent chest clapping but add in gravity-assisted positions if appropriate. Your physiotherapist will be able to advise you.
Begin blowing games and huffing as soon as possible. Children should be taught "The Active Cycle of Breathing Technique" (ACBT) as soon as they are old enough. This is a combination of deep breathing exercises (during which time clapping or shaking may be added), breathing control (relaxed breathing) and forced expirations (huffing). This technique is the basis of most treatments and can be performed in all positions. Physiotherapy devices can be added to improve effort and/or feedback.
8 years and upwards
If appropriate, gradually progress towards independent-BUT-supported treatment. During a chest infection, “hands on” techniques may still be helpful. It may also be useful to add in a physiotherapy device such as the PEP, Flutter® or Acapella® these devices can sometimes help with adherence if physio is becoming difficult.
Teenagers
New techniques/strategies may be introduced to help your teen fit their physio around busy school/college and social timetables and make them more independent with their physiotherapy. Physio devices (as above) may be helpful.
Learning a new breathing technique such as modified autogenic drainage may also be useful.
Your teen can ask their physio for advice if they are finding it difficult to fit physio into their daily routine.
How often?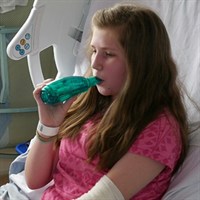
People with PCD often need to do chest physiotherapy twice daily, which usually lasts around 15 minutes and more frequently or for a longer duration during a cold or chest infection when there are more secretions than usual. During these times physio may change to be more intensive to help clear your child’s chest effectively.
Adjuncts to physiotherapy
A variety of equipment can be used to aid clearing secretions from the lungs and the physiotherapist will teach you the technique that is most suitable.
Lots of children with PCD also use inhalers and/ or nebulisers (mist-like liquid medications) to optimise their chest clearance. These can help to ensure that secretions are easily moved and make your physiotherapy as effective as possible. This will also be reviewed in clinics to see if this is something your child would benefit from.
Exercise and posture
An active lifestyle is important and regular exercise should be strongly encouraged.
Treating your sinuses
Patients with PCD can also have issues with their sinuses and upper airways becoming persistently congested and/or runny. There are a number of options for treating this; if your child is approx. 8 years old or older they may be introduced to sinus rinsing. This is a process using normal saline to help clear your sinuses to prevent/ alleviate the build up of secretions which can lead to infections and result in sinus headaches – which have a great impact on quality of life. This can also help to improve hearing and the sense of smell.
This technique can be introduced in clinic or during a hospital stay and is recommended to be done at least once a day to help clear your sinuses and help stop infections before they go to your chest. Your child will also be assessed by a specialist ENT (ears, nose & throat) doctor during our larger clinics or at your local hospital to assess for any other upper airway issues.
Providing a sample
During every clinic visit, the physiotherapist will ask you to provide a sputum sample or, for little ones unable to cough up, take a cough swab (coughing or huffing onto a long cotton-bud like stick). This is then sent for analysis to check for any harmful bacteria in your child’s airways that may need treating with antibiotics. These usually take around five days to process and you will be contacted if you need to make any changes to your medication.
Knowing that we have different bacteria in our noses/sinuses to our chest, if your child is old enough we will use the sinus rinsing to obtain a sample of fluid that has passed through the sinuses to send for analysis. If your child is too young for this, a swab can also be taken from the inside of your nose for the same investigations.
Home and school visits
If your child is under the care of Royal Brompton Hospital, we may be able to offer you a home or school visit to help discuss PCD in greater depth than we are able to in clinic. We can review your physiotherapy techniques at home and any issues that may arise.
We can also make contact with your child’s school or nursery to help explain about the impact of PCD and what they can expect. These visits are usually with both a specialist PCD physiotherapist and a PCD clinical nurse specialist so we can offer as much support and information as possible. If you feel this would be beneficial, please speak to either the physiotherapist or nurse in clinic.
