Speech and language therapists support babies and children with eating, drinking and swallowing difficulties.
The team will assess your child and will provide advice and strategies to help support your child to have safe, efficient and pleasurable eating and drinking experiences.
Jump to section:
- Feeding and swallowing assessment
- Managing mealtimes
- Non-nutritive sucking
- Speaking valve assessment
- Tips for thickening drinks
- Tracheostomy
- Videofluoroscopy swallow study
- Contact us
Feeding and swallowing assessment
![]() If your consultant has any questions or concerns about your child’s eating, drinking or swallowing, they can make a referral to our service.
If your consultant has any questions or concerns about your child’s eating, drinking or swallowing, they can make a referral to our service.
The reasons for referring may include concerns about:
- Food or drink "going down the wrong way" when swallowing, causing respiratory symptoms, such as chest infections, persistent coughing etc
- Coughing or choking on food or drinks
- Infants who are getting tired or breathing fast and getting sweaty when drinking
- Infants who are not drinking or eating enough to gain weight
- Infants and children who avoid eating and drinking certain consistencies or textures
The speech and language therapy (SLT) team see children in all areas of the hospital as inpatients, outpatients and day case admissions. The assessment process is similar for all patients:
- Case history: the SLT will ask you a range of questions about your child’s feeing history from birth to the current day
- Assessment: the SLT will observe your child eating as per their normal diet, but also will be particularly interested in seeing them eat any foods or drinks that they find more challenging
- During the assessment: the SLT will observe closely and may also place a small stethoscope on your child’s neck in order to listen for sounds associated with swallowing
- Recommendations: after the assessment the SLT will discuss the findings and make recommendations for either:
- Strategies to improve your child’s feeding or swallowing
- Further assessment of swallowing using a test called a videofluoroscopy
If your child has been referred for a SLT assessment and you have any further questions about what to expect, please call us
Phone: 020 7351 8369
Managing mealtimes - supporting your child's eating
 Mealtime setting
Mealtime setting
- Aim for a positive, calm eating environment.
- Try to avoid becoming stressed, angry or upset in response to your child’s feeding behaviour
- Having regular mealtimes and a routine (e.g. putting plates on the table / sitting at the table) helps your child know it is time to eat
- Encourage your child to sit in a high chair / at the table
- Try to eat together – this is more sociable, and your child learns from watching you eat
- Avoid using distractions to get your child to eat
- Try to follow your child’s pace – learn to pay attention to his/her signals e.g. slow down or speed up – this will help your child to feel more in control
Food types and volumes
- As your child gets older they will need less milk and more solids. A common reason for children to eat small volumes of solids is if they take too much milk.
- Offer food based on your child’s preferences. For example, short frequent meals if they like to eat little and often, or three larger meals a day, if this is how they eat best.
- Encourage your child to feed themselves. This gives them more control at the mealtime and may help with their intake.
- Consider your child’s age and development when offering food textures. They may not eat if they find the foods too hard to manage.
- Offer portion sizes that are manageable for your child.
- Offer a variety of food types, tastes and textures across meals and across the day.
Managing your child’s eating behaviours
- Be specific – praise them for behaviours you want them to do, such as
- sitting down
- using their spoon
- eating
- finishing their plate
- eating a certain food
- Praise even small, good behaviours
- Ignore unwanted or undesirable eating behaviours
- Avoid focusing conversation on each bite or mouthful that your child does or does not eat
- Be consistent, and make sure other people are doing the same
- Avoid using food-based rewards for eating e.g. "If you eat this carrot, you can have ice cream"
- You can use other reward systems e.g. sticker charts or play after eating for achieving desirable mealtime behaviours or eating
Non-nutritive sucking
What is non-nutritive sucking?
Sucking without swallowing any milk, like sucking on a dummy.
Why is it recommended for my baby?
When your baby is unwell and in hospital, they may not be able to suck their feeds. They may have milk given via a tube direct into their stomach.
Non-nutritive sucking may be recommended because:
- It helps the baby to settle and be calm. For this reason, it is often used during medical tests, like an ECHO or blood tests.
- Sucking gives your baby a positive experience in their mouth and gives opportunities to practice skills needed for later feeding, and maintains skills they have already learnt.
- If your baby is on CPAP, sucking can help provide a good seal in the mouth and maximise the delivery of the CPAP to your baby.
How to practice non-nutritive sucking
On an empty breast:
- Make sure you have expressed recently so that your breast
is empty - Hold your baby in a breastfeeding position, skin to skin
if possible - Let your baby suck on the empty breast
Dummy or finger:
- Cuddle your baby
- Offer a dummy or your clean finger
- Be patient, your baby may need a few tries to get used to sucking again
When to practice non-nutritive sucking:
- Offer at the beginning of a tube feed, until baby falls asleep / stops sucking
- Offer when baby is unsettled or uncomfortable
- Offer when baby is awake and sucking on their lips or hands
Speaking valve assessment
What is a speaking valve?
A speaking valve is a one-way valve that is attached to the end of the tracheostomy tube. It opens to allow air in through the tracheostomy during a breath in and then closes on the breath out, directing the air up through the larynx and out of the mouth in order to produce voice.
There are a range of different speaking valves available and speaking valves can be used within a ventilator circuit and with oxygen.
Can all children have a speaking valve?
Not all children are suitable to have a speaking valve. Your child must have adequate space for passage of air up and around the tracheostomy and above it.
There are some key pieces of information and questions that the SLT will ask before the assessment to establish if your child is suitable for a trial:
- What is the reason that your child has a tracheostomy? (specifically is it due to closed vocal cords or blocked upper airway?)
- What were the results of your child’s last ENT assessment?
- How old is your child and what size is their tracheostomy tube?
- Does your child make a sound when they cry?
- Does your child make any sounds or words?
- Does your child have a cuffed trachestomy tube and can they tolerate the cuff down?
- How much suctioning does your child need? Do they have difficulties with oral or tracheal secretions?
If a trial is not felt to be appropriate at this stage, or if your child is not able to tolerate a speaking valve, this can be reviewed again in the future. The speech and language therapist will still be able to support your child with ideas for voice and communication development without a valve.
The assessment
If your child is a suitable candidate for a trial of a speaking valve an assessment will be carried out at the Royal Brompton Hospital. The SLT and another team member will carry out the assessment. The steps are as follows:
- An assessment of your child’s normal breathing will take place with oxygen saturations if appropriate
- Your child will be placed on an oxygen saturation monitor for the assessment
- You may be asked to suction the tracheostomy before the assessment
- Depending on the age of your child you will be asked to engage with them in an interesting activity before and during the trial
- The first stage of the trial will be for the tracheostomy to be covered with a gloved finger to see if air flows through the mouth or nose or becomes blocked up behind the finger
- If this is tolerated then the valve will be placed on the end of the tracheostomy
- Your child will be closely monitored to assess their tolerance of the valve and if tolerated a plan will be made for further trials over the course of your assessment visit
- If the valve is tolerated then a plan for going home and building up your child’s tolerance of the valve will be discussed with you
Tips for thickening drinks
Why do we thicken liquids?
Any liquid can be thickened to:
- Prevent drink going down the wrong way (onto the lungs), as this can cause chest infections
- Develop oral skills such as lip and tongue movements
Who should know about my child’s thickening requirements?
Anyone who may be feeding your child, for example family members, carers, nursery school staff, medical staff
What consistencies are available?
There are three consistencies:
Stage 1 - syrup (thin)
- Drunk using a straw, beaker, or cup, or a bottle (may need a medium-flow teat)
- Runs off the spoon leaving a thin coating
Stage 2 - custard (thick)
- Drunk from a bottle (may need a fast-flow teat), beaker, or cup
- Drips off the spoon leaving a thick coating
Stage 3 - pudding (very thick)
- Fed using a spoon (may not be able to be drunk from a bottle, beaker, or cup)
- Stays on the spoon with only occasional drips
Your speech and language therapist will advise you on which consistency to use.
Preparation
- Use the amount specified on the tin for syrup/custard/pudding consistency
- Vigorously shake/stir the powder and liquid together for approximately one minute and leave to stand for a few minutes
- Some thickeners work best if you put the powder in first and then add the liquid
- Drink immediately and discard any leftover liquid
Tracheostomy
What is a tracheostomy?
A tracheostomy is an artificial opening in the trachea (windpipe). A tracheostomy tube can be inserted into the opening. Air is directed in and out of the tracheostomy tube and not through the nose and mouth, which is what usually happens.
There are a number of different reasons why a child may need a tracheostomy. They may include a narrowing in the airway making breathing difficult, or it could be due to a lung condition that requires long-term ventilation, which is delivered via the tracheostomy.
Eating and drinking with a tracheostomy tube
Having a tracheostomy tube will not necessarily affect a child’s eating or drinking. However, every child is different and each will respond in a different way. If your child has a new tracheostomy, a feeding and swallowing assessment by a speech and language therapist is recommended.
Communicating with a tracheostomy
The presence of a tracheostomy tube means that air will come in and out of the tube, bypassing the throat, vocal cords and nose and mouth. As air will not pass through your child’s vocal cords, your child will not be able to make a voice (sounds).
Voice is the sound of speech only. Your child may try and say words or cry but no sound will come. There are a number of other ways your child can communicate. They include signing or gestures or a speaking valve. A speech and language therapist will advise you how best to support your child’s communication.
Videofluoroscopy swallow study
What is a videofluoroscopy?
It is a video X-ray test that looks at your child's eating, drinking and swallowing.![]()
Why has my child been referred for this test?
This test gives a clearer picture of what is happening inside your child’s mouth/throat when he/she is eating, drinking and swallowing.
It also shows us where food and liquid goes when your child swallows. It will give us much more information on your child’s swallowing process and allow us to diagnose and then treat any problems.
Does the test hurt?
No. The test is totally painless. It does not involve any needles or tubes, and we will try to feed your child as closely as possible to how he/she feeds at home.
Some children may be nervous because the X-ray is an unfamiliar experience, or because the room is a strange place. It might help to show the pictures on the right to your child beforehand to help him/her to know what to expect.
We have a DVD player and children's DVDs to help to keep your child entertained and relaxed while they are waiting for the test to start. If you think your child will enjoy this and co-operate better, please notify the speech and language therapist (SLT) so we can make sure the DVDs are available.
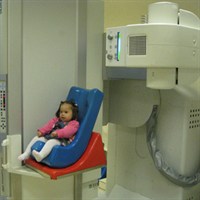 What does the test involve?
What does the test involve?
Your child will be seated in a small supportive chair next to an X-ray machine. He/she will be given different types of food or drink to swallow. This will be mixed with or coated with a liquid which makes the food and drink visible in the X-ray and so let us look at your child’s swallowing process. We record the images to keep for our records.
We try to follow the child’s usual feeding routine as closely as possible. This means if you usually feed your child, we will ask you to feed him / her during the test.
What do I need to bring with me to the appointment?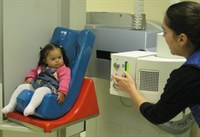
You should bring some food and drink that your child usually eats. It is also helpful if you bring your child’s usual bottle/spoon/beaker/cup or cutlery.
If your child requires special positioning or seating during mealtimes, please let us know and please bring the seating with you, if possible.
How do I prepare my child for the test?
You can feed your child before the assessment. However, we advise that only a small amount of food is eaten as your child will need to eat and drink during the test. This is easier if your child is hungry.
Who will be involved in the test?
- A parent / carer
- Your child
- A speech and language therapist (SLT)
- A radiologist (doctor)
- A radiographer
Are there any significant risks or side effects?
Radiation can be harmful in large doses. However, a very low dose of radiation is used for the X-rays. We take every precaution when using radiation.
If you are pregnant, or think you may be pregnant, you will need to stay outside of the X-ray room during your child’s test. This is because radiation, even in small doses, can cause harm to unborn babies.
Any other children with you will not be allowed into the X-ray room during your child’s test. This is due to the small risk of harm from radiation. Please make alternative arrangements for your children.
Aspiration (when food or drink goes "down the wrong way" into the windpipe) can happen during the test. We limit the degree to which this occurs as much as possible.
Please remember that we would not recommend this test if we did not believe the benefits outweighed any potential risks. The SLTs are happy to discuss any concerns you may have about the test.
When will we receive the results?
Whenever possible we will tell you the results of the test immediately afterwards. Sometimes further analysis of the test may be necessary. In this case we will arrange a time to contact you with the results. The test is recorded and we can show you the images to explain any difficulties your child has. If there are any changes needed to your child’s current eating and/or drinking pattern, these will be discussed with you and the medical team involved in your child’s care.
Where will the test take place?
The videofluoroscopy will take place in the imaging department (X-ray) on the 3rd floor of the Sydney Street building.
Contact us
Call us if you would like to speak to a speech and language therapist or have any questions about the services we provide.
Phone: 020 7351 8369
